Total knee replacement is an increasingly common operation across the world with nearly 4-500,000 procedures performed in the United States annually many using Makoplasty. The profile of patients undergoing this operation has changed over the years along with who is an operative candidate. We see many patients now who are very high demand and wish to engage in physically demanding activities after surgery. Many patients are no longer willing to give up activities which stress knee replacement implants. Thus, today’s knee replacement procedures need to offer higher demand solutions that will provide comfort, stability and durability under uses and abuses to which patients subject these implants. The historical 20% dissatisfaction rate that patients have reported after total knee is no longer acceptable given modern patient demands. It is incumbent upon surgeons and engineers to continue innovating implants and surgical technique to address these demands and raise the bar on patient satisfaction and expectations.
Makoplasty is considered a surgical robot. These have received much attention lately. The definition of a robot is a physical object, programmable by a computer than perform tasks autonomously. In fact, surgical robots are not yet autonomous and require human constant human input. There are, to date merely extensions that help guide and improve the accuracy of human movement. In the case of the Makoplasty, the device is a non-autonomous cutting and milling machine that helps determine the optimal position of the knee implant and then assist surgeons in placing the implant accordingly.
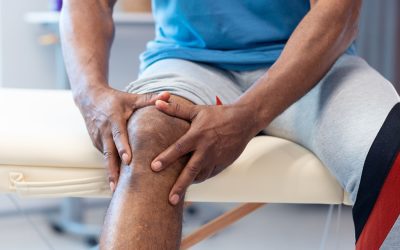
Several points should be clarified about the Makoplasty knee replacement. First, it is not minimally invasive surgery as often marketed. For the “robot” to be registered to the patient’s anatomy, trackers must be drilled into bone of both the tibial and femur. These trackers help the robot communicate with the surgeon during placement of the implant. The white dots in the picture to the right show the trackers drilled into the bones away from the knee joint. This is not necessary with conventional total knee replacement.
Second, while the Makoplasty can help customize the placement of the implant relative to the patient’s anatomy, it is not a custom implant. In fact, the Stryker Triathlon knee system used with the Makoplasty was designed and released in 2005 with no system updates since that time. It has only 8 average “off-the-shelf” sizes. Compare this to more modern implant systems that have up to 14 sizes to better fit variations in anatomy. Stryker alleges that the robot can assist surgeons in fitting the implant to the bone; but if the implant does not inherently fit due to size mismatch, alterations in the implant position to optimize fit may negatively affect function.
The Conformis patient-specific total knee, on the other hand, is a truly customized knee replacement. Each implant is custom designed for each patient. The shape and fit are optimized to fit the bone, minimize bone removal and ensure optimal implant placement. Like the Makoplasty, computer algorithms can be used to determine the best position for the implant to replicate patient anatomy. Unlike the Makoplasty, the customized implant does not rely on a generic shape but replicates the patients normal bone shape so that the knee functional in a more kinematically normal fashion.
The 3-D printed cutting blocks used in the Conformis total knee are low profile allowing a truly minimally, quad sparing approach. No additional holes need to be drilled into the bones. The image to implant technology also reduces inventory needed for each case and reduces the number of instruments that need to be sterilized. This theoretically can reduce the infection risk and improve the efficiency of the case.
Dr. Parsons has used by the Stryker Triathlon and Conformis knees extensively over a course of many years. While any implant can provide an excellent outcome when properly placed, his experience has proven the merits of the Conformis knee leading to his preference for this system over the Makoplasty technology. Dr. Parsons recounts that, having given numerous community education lectures over a period of years, patients who learn about the differences between these technologies often ask why every surgeon does not use a truly customized, patient-specific implant.
The debate is actually quite transparent. If you could have an 13 year old, off-the-shelf implant placed with the assistance of a device that is not a true robot and requires additional holes drilled in the bone, or a customized minimally implant designed with 3-D printing to ensure optimal placement, which would you rather have?